How Your Menstrual Cycle Works
Your menstrual cycle is more than just your period—it’s a dynamic, intricate process that reflects your overall health and hormonal balance. Understanding how it works is key to optimizing your well-being, fertility, and energy levels. This guide breaks down the three interwoven cycles within your menstrual cycle, explains each phase, and highlights why tracking your cycle is one of the most powerful tools for self-awareness.
Three Cycles In One
You may or may not already know this, but your menstrual cycle is composed of three distinct but interconnected cycles.
Each of the three cycles—the hormonal cycle, the ovarian cycle, and the uterine cycle—is intricately connected, working in harmony to regulate menstruation, ovulation, and overall reproductive health. Let’s dive deeper into the physiological mechanisms that drive each of them.
1. The Hormonal Cycle: The Master Regulator
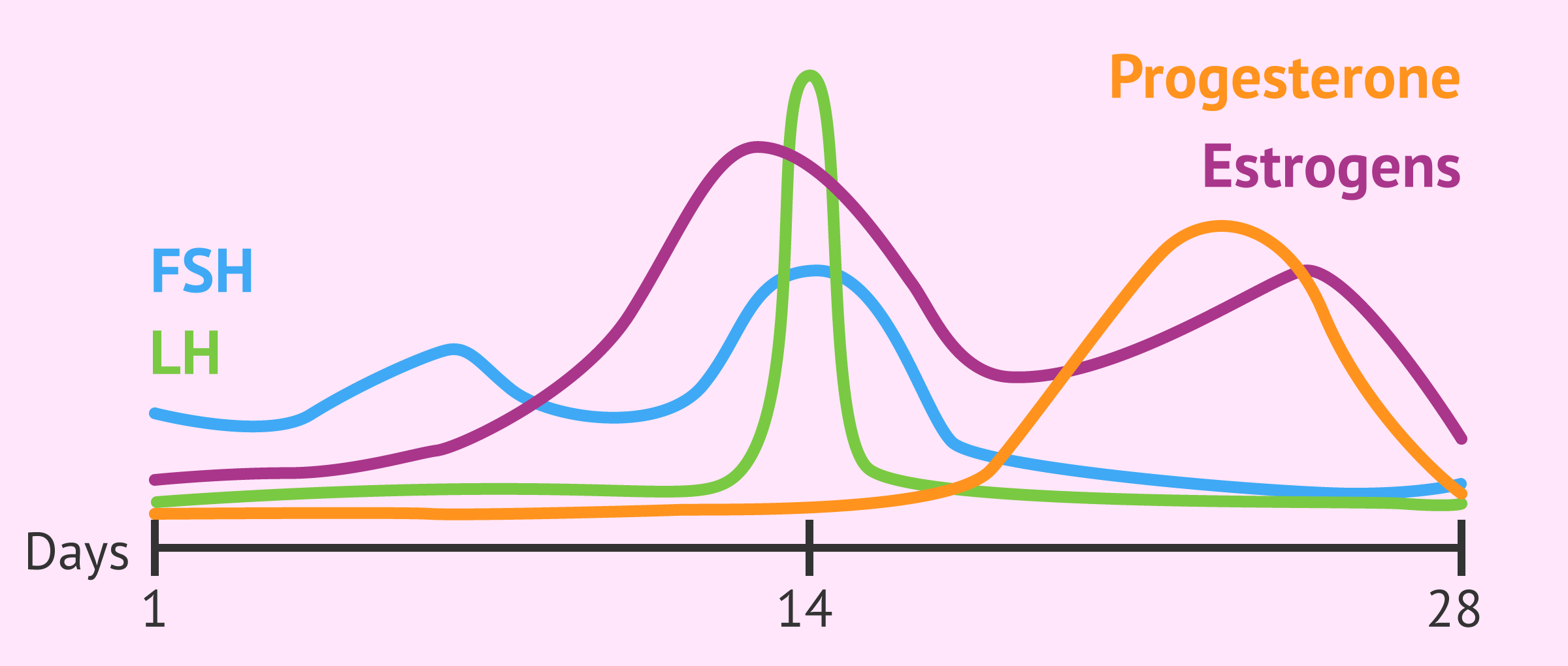
Hormones are your body’s messengers and the conductors of your menstrual cycle, orchestrating every shift and transition. The hormonal cycle is governed by the hypothalamic-pituitary-ovarian (HPO) axis, a communication network between your brain and ovaries. This axis regulates hormone production through negative and positive feedback loops, ensuring that each phase transitions smoothly. The main players include:
Follicle-stimulating hormone (FSH), released by the pituitary gland, kicks off the cycle by stimulating follicle growth in the ovaries.
Estrogen, primarily produced by the developing follicles, plays a critical role in both the ovarian and uterine cycles. Rising estrogen levels signal the hypothalamus to reduce FSH and prepare for ovulation.
Luteinizing hormone (LH) surges mid-cycle, triggering ovulation.
After ovulation, progesterone takes the lead, secreted by the corpus luteum to prepare the uterine lining for potential implantation.
Beyond fertility, estrogen and progesterone impact neurotransmitters like serotonin and dopamine, influencing mood, energy levels, and even cognitive function throughout the cycle.
The hormonal cycle is an intricate and carefully timed dance between FSH, Estrogen, LH and progesterone.
2. The Ovarian Cycle: Follicular Selection and Ovulation
The ovarian cycle consists of follicular development, ovulation, and the luteal phase. Here is an overview of what happens in each stage of the process:
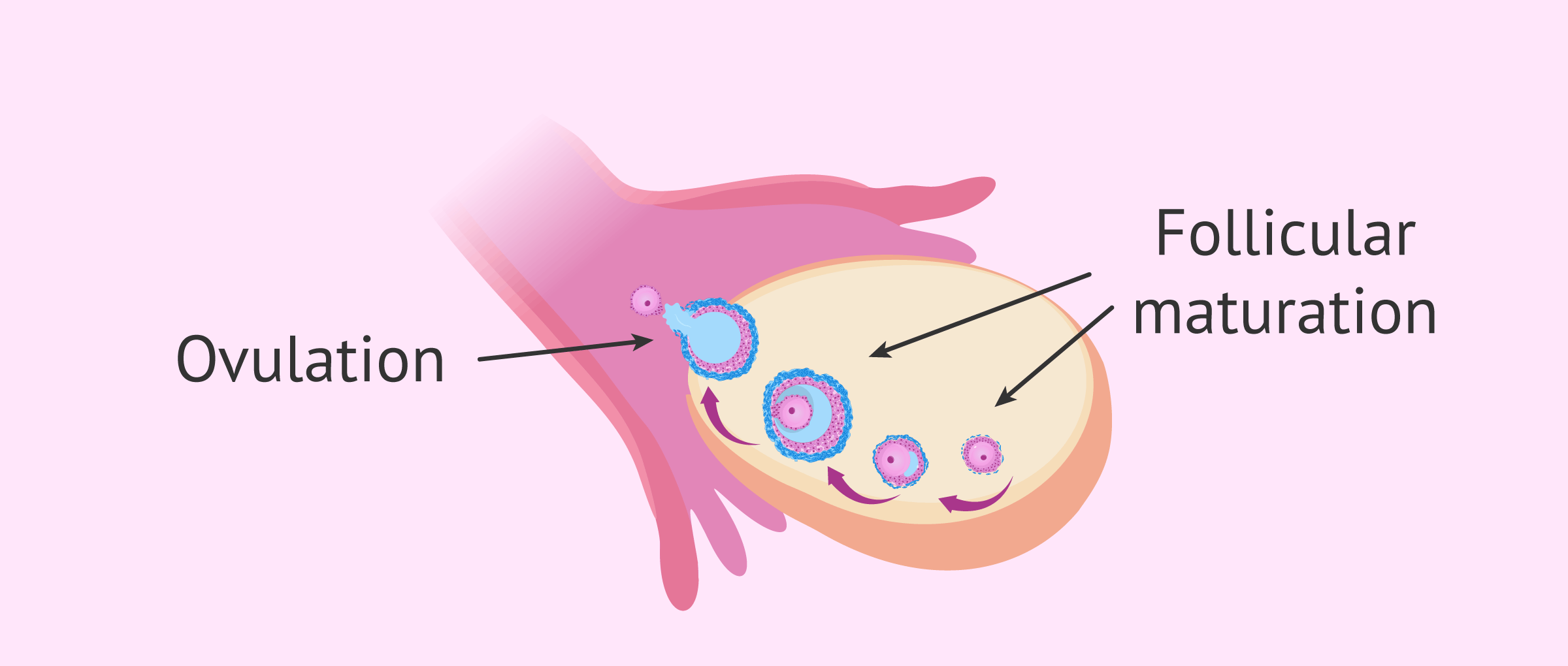
Early follicular phase (Day 1 of your period to around Day 7): In the ovary, several follicles (each with a tiny egg inside) begin to develop under the influence of FSH. One becomes the dominant follicle - the candidate to be released. The selection of this follicle depends on its FSH receptor sensitivity and its ability to produce estrogen. During this phase, a positive feedback loop occurs: the release of FSH stimulates to the release of estrogen, which in turn leads more FSH and more estrogen (you get the gist)…. until the dominant follicle is mature enough to be ovulated and…
The positive feedback loop between FSH and Estradiol (a form of estrogen) continues until one of the follicles is ready for ovulation (dominant follicle).
Ovulation: This peak in estrogen triggers a surge of LH, which causes the dominant follicle to rupture and release the egg. The process of ovulation is inflammatory in nature, involving enzymes like plasmin and prostaglandins that help break down the follicular wall. The rupture itself is a micro-inflammatory event, which is why some women experience mittelschmerz, a mild ovulation pain. Contrary to popular belief, this is the most important part of the cycle - not the bleeding. The egg is now in the Fallopian tube, awaiting the arrival of sperm to fertilize it… or not. The egg lives only for 12-24hs (yep, you are only fertile for maximum a day during your whole cycle!), so if that sperm does not appear, it will simply disintegrate and be reabsorbed.
During ovulation, one of the mature follicles ruptures and the egg inside it is released.
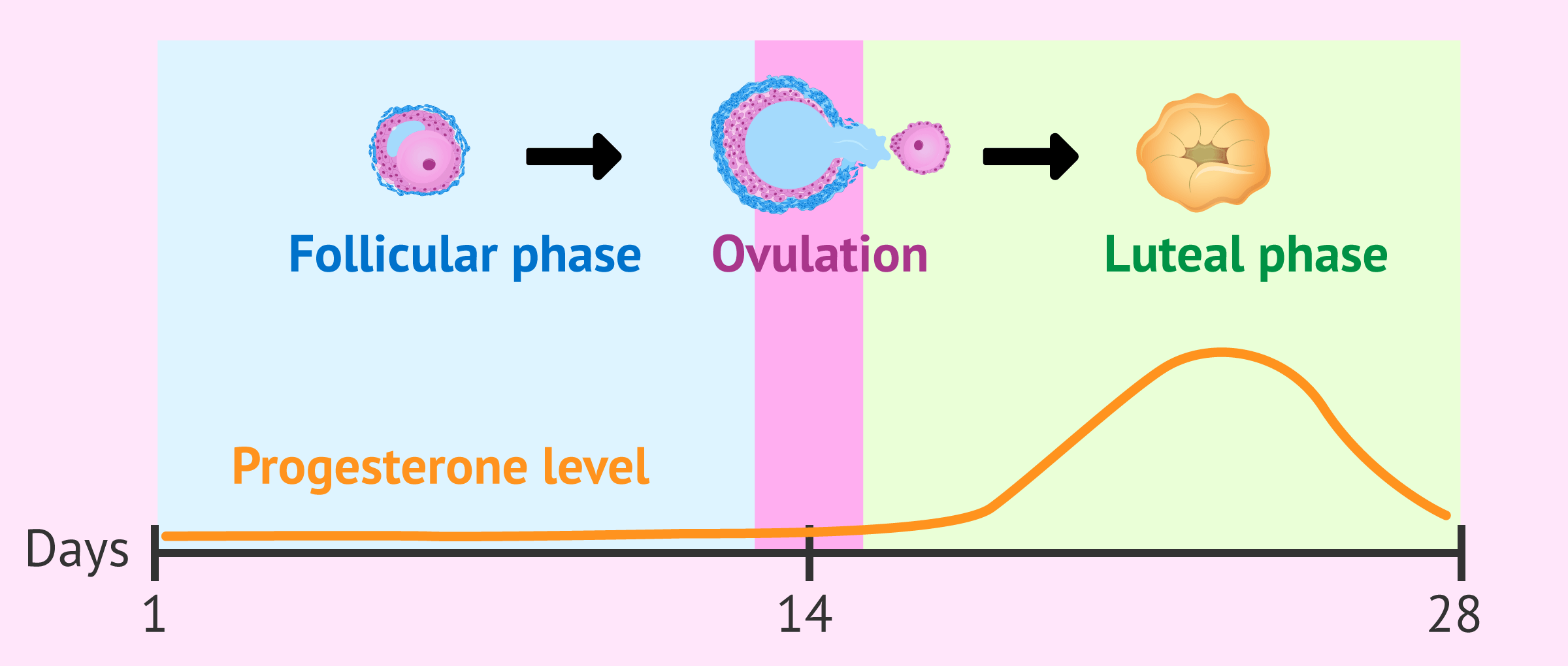
Luteal phase: Meanwhile, the ruptured follicle (the little balloon where the egg was housed while in the ovary) transforms into the corpus luteum, a temporary endocrine structure that secretes progesterone. Why? Because we need progesterone to help develop the uterine lining to sustain a potential pregnancy. If fertilization occurs and the blastocyst successfully implants into the inner wall of the uterus, the production of progesterone continues. If fertilization doesn’t occur, the corpus luteum degrades after 12-16 days (the duration of your luteal phase is determined by the life spam of the corpus luteum), leading to a drop in progesterone. This sudden drop in progesterone (and estrogen) lead to the start of menstruation. And the cycle begins once again.
After ovulation, the remains of the follicle left behind in the ovary become the corpus luteum, a temporary endocrine structure that secretes progesterone during luteal phase. (Corpus luteum, luteal phase… get it?)
3. The Uterine Cycle: Preparing for Pregnancy or Resetting
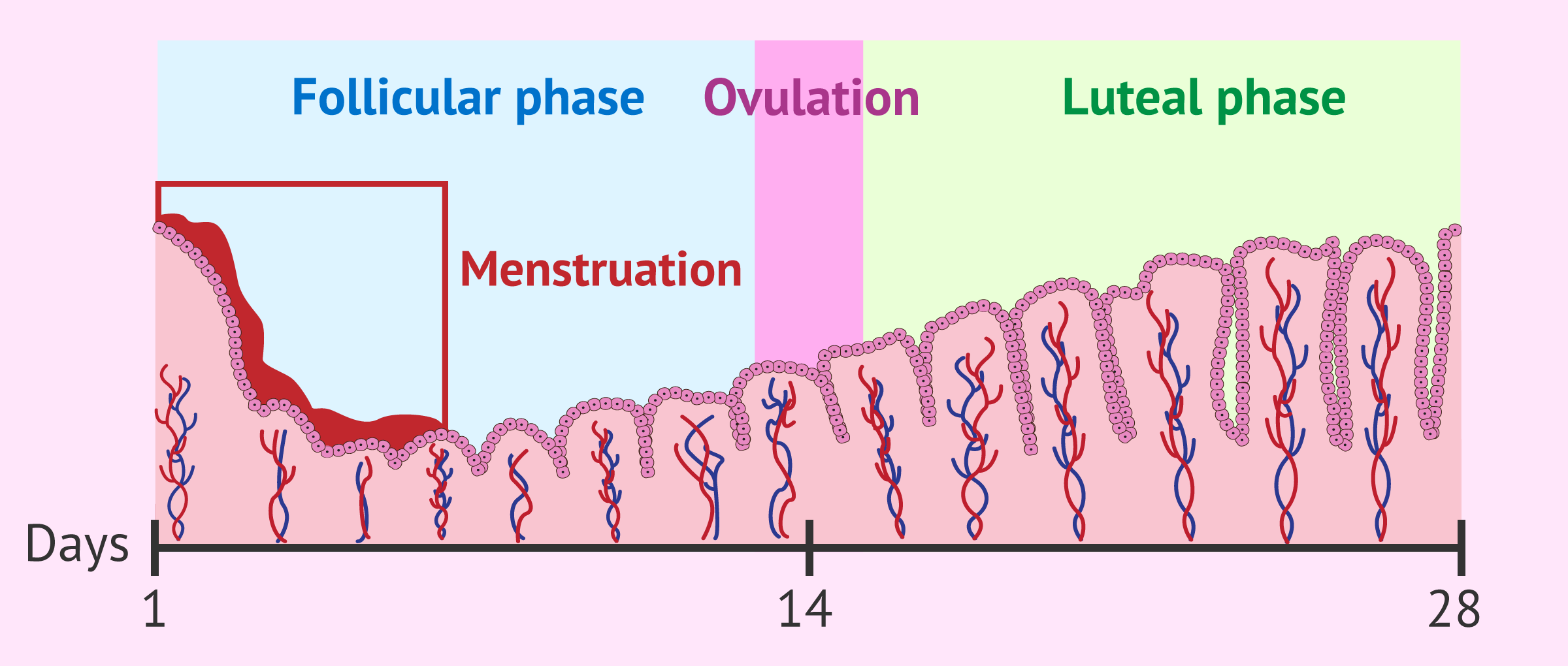
The uterine lining (endometrium) goes through proliferative, secretory, and menstrual phases, responding to the same estrogen and progesterone fluctuations present in the other two cycles. Here is what happens in each phase…
The uterine lining also goes through lots of changes throughout the cycle!
Proliferative phase: This phase coincides with the follicular phase, when the follicles are developing and the FSH/Estrogen feedback loop is full blast. Estrogen stimulates endometrial thickening and increased vascularization to the area. The uterus slowly starts to prepare…
Secretory phase: When we get to the luteal phase, the progesterone released by the corpus luteum stabilizes the endometrium, making it receptive to the potential implantation of an embryo and reducing uterine contractions to prevent premature shedding. But more often than not, the sperm never arrives, the egg is never fertilized and the embryo never implants…
Menstrual phase: As you read above, if no implantation occurs, progesterone levels drop when the corpus luteum dies, which triggers inflammatory cytokines and prostaglandins, leading to vasoconstriction and the shedding of the uterine lining. In plain English: the lining of the uterus can no longer hold itself up, and it sheds in a natural inflammatory process called menstruation.
This may sound like a lot, but I hope the images help! As you can see, all three cycles work in tandem and are deeply interconnected. All that is happening in your body right now! Isn’t it fascinating?!
Here you can see how all three cycles align. Note that these images show a 28 day cycle for illustrative purposes, but your cycle might be longer or shorter, your ovulation might happen earlier or later.
Ovulation: The Main Event of Your Cycle
Many people mistakenly think their period is the most important part of the cycle, when in reality ovulation is actually the pinnacle of the whole menstrual cycle. Without ovulation there is no corpus luteum, so no progesterone is produced, leading to hormonal imbalances and cycle irregularities. And of course, if you are not ovulating (which you can only confirm through an ultrasound, an LH test or by tracking your cycle) there is no possible way for you to get pregnant - naturally, at least. But even if you’re not trying to conceive, ovulation is a sign of hormonal balance and systemic health essential for:
Bone health
Progesterone stimulates osteoblasts, the bone-building cells responsible for maintaining and increasing bone density.
Estrogen supports calcium absorption and prevents excessive bone resorption (when bones break down). Without regular ovulation, estrogen and progesterone levels can become imbalanced, increasing the risk of osteopenia or osteoporosis over time (and none of us want that!).
Women with anovulatory cycles (cycles where ovulation does not occur) or conditions like functional hypothalamic amenorrhea often experience lower bone mineral density, even at a young age.
Example: In athletes with low energy availability or excessive training, lack of ovulation contributes to the Female Athlete Triad, a condition that includes menstrual dysfunction, low bone density, and energy deficiency.
Mood stability
Progesterone is a precursor to allopregnanolone (ALLO), a neurosteroid that enhances GABA receptor activity in the brain, leading to a calming, anti-anxiety effect.
Women who do not ovulate regularly may experience increased anxiety, irritability, and mood fluctuations, particularly in the second half of their cycle.
A lack of progesterone can also contribute to premenstrual dysphoric disorder (PMDD), a severe form of PMS linked to mood instability.
Example: Women who come off birth control after years of anovulatory cycles often experience mood fluctuations as their brain adjusts to natural progesterone production for the first time in years. You can read more about what the birth control pill does, and doesn’t do, in this article.
Metabolism regulation
Progesterone increases body temperature, slightly raising basal metabolic rate (BMR) in the luteal phase. This helps regulate energy expenditure and can affect appetite and nutrient partitioning.
Regular ovulation supports insulin sensitivity—women with anovulatory cycles (such as in PCOS) often experience higher insulin resistance and dysfunctions in blood sugar regulation, leading to metabolic challenges.
The hormonal shifts around ovulation also influence fat and carbohydrate metabolism, optimizing the body's ability to switch between fuel sources efficiently and improving metabolic flexibility.
Example: Women with irregular ovulation may struggle with unexplained weight fluctuations, cravings, or energy dips due to disrupted metabolic function.
Remember:
you can still bleed regularly even if you are not ovulating!
The fact that you have a regular period does not confirm ovulation!
Why Tracking Your Cycle Matters
Understanding this at play in your own body is the key to working with your cycle, and not against it. Tracking your cycle can reveal endocrine, fertility, mood, metabolism, and even immune function patterns.
Want to learn exactly how to track your cycle and interpret these hormonal shifts?
In VITAL I teach you everything you need to know to accurately use the Symptothermal Method to decode your body’s signals and take charge of your fertility, energy, and overall health.
How to Get Started
If you want to gain a deeper understanding of your cycle and fertility, the Symptothermal Method is the most powerful tool. In VITAL, you’ll learn how to track your basal body temperature and cervical mucus to:
✅ Optimize fertility awareness (for conception or pregnancy prevention)
✅ Identify ovulation (confirm a healthy luteal phase and adequate progesterone levels)
✅ Spot sings of hormonal imbalances before they become health issues (such as irregular cycles or heavy periods)
✅ Optimize exercise, work, nutrition, and lifestyle habits based on the phase of your cycle (live in sync with your cycle)
Cycle tracking is about…
taking control of your fertility,
reclaiming your connection with your body,
and living in alignment with your natural rhythms.